Autonomic dysreflexia is a medical condition that may occur in some people with spinal cord injury. Learn more about the warning signs and symptoms of this issue.
Autonomic dysreflexia is a serious medical condition that some people with a spinal cord injury may be susceptible to, depending on your injury's location and severity. This issue can result in medical emergencies such as stroke, seizure, or cardiac arrest.
It can happen when there is a hyperactive reflex in your body's autonomic nervous system—a control center for key functions like breathing and digestion—to something happening below the point of damage in your spine. It is an overreaction of your body that can lead to a dangerous scenario if not quickly resolved.
Although it's not as common as other post-spinal cord injury medical issues, it's vital that you and your caregivers understand how autonomic dysreflexia works and its warning signs, especially if your injury is located at T6 or above. Once you and your team are on the lookout for symptoms that indicate you may be experiencing this condition, you'll all know what to do to resolve it promptly.
Common symptoms of autonomic dysreflexia
Initially, the most typical signs that you may be experiencing this serious issue are subtle. They include a flushed feeling and an intense headache. Other more innocuous warning signs are heavy sweating, a stuffy nose, or chills (without a fever).
Additional symptoms may include:
· Slowed heart rate
· Fuzzy vision
· Difficulty breathing
· Muscle spasticity
· Bowel impaction
· Goosebumps
· Blotchy skin
· Cold, clammy skin below the level of injury
You may also experience mental warning signs that mimic the body's response to stress. These include a feeling of anxiety, apprehension, or restlessness. You may experience some confusion as well.
Any of these symptoms of autonomic dysreflexia can come on quickly and without warning. It's vital to stay vigilant, pay close attention to what's happening with your body, and take swift action.
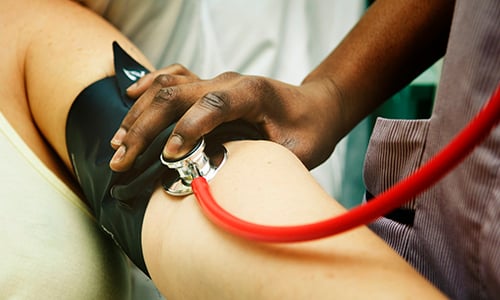
Check your blood pressure
As you can see, some symptoms of autonomic dysreflexia can mimic other common and more minor medical conditions, such as a cold or allergies, or even a stressful day. That's part of the inherent danger of autonomic dysreflexia—the warning signs may lead you or your caregiver to believe it's something less menacing when, in reality, you and your team need to act quickly to a potentially life-threatening medical issue.
One of the keys to distinguishing true warning signs from something else is checking your blood pressure. Since autonomic dysreflexia results in a noticeable spike in your blood pressure, it's important to have a home blood pressure monitor handy for you and your helpers.
Some general blood pressure reading guidelines:
· If your injury is above T6, often your normal systolic blood pressure is in the 90–110 mm Hg range
· If you have a reading of 20-40 mm Hg above baseline, it may be a sign of autonomic dysreflexia
· For adolescents, a reading 15-20 mm Hg above baseline is a symptom
· For children, 15 mm Hg above baseline potentially indicates autonomic dysreflexia
When to seek medical attention
Suppose your blood pressure is higher than normal in combination with some of the symptoms above. In that case, you'll need to find the cause of your autonomic dysreflexia and resolve it quickly, if possible. It may be something as simple as loosening tight clothing or getting the kinks out of a blocked catheter. Continue to check your blood pressure every 5 minutes.
More serious causes that warrant a trip to the ER may be fractures or broken bones, or any other trauma that could be at the root of the problem. If you or your team are unable to identify the cause, seek medical attention immediately.
References: