Autonomic dysreflexia is a rare but serious medical condition that may afflict some people with spinal cord injury. Learn more about this potentially life-threatening condition.

After a spinal cord injury, it's important that you are aware of your vulnerability to certain medical conditions. Your medical team may have informed you of common dangers such as burns, pressure sores, and muscle spasms. However, there is a lesser-known medical problem unique to many people with a spinal cord injury that is serious and can be life-threatening.
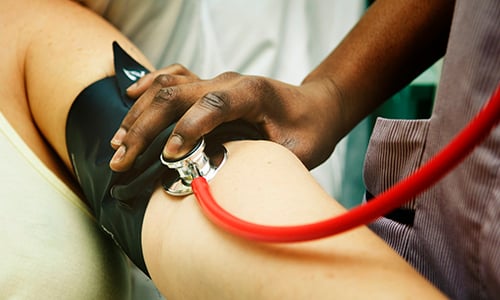
It's called autonomic dysreflexia, or AD, and it can cause a sudden spike in your blood pressure in combination with extremely low heart rate. This dangerous scenario can lead to a seizure, stroke, or cardiac arrest. Autonomic dysreflexia (also known as autonomic hyperreflexia) should be considered an emergency with the need for immediate medical attention.
Understanding autonomic dysreflexia and the fast-acting impacts on your body is important not only for you but also to caregivers, family members, and other people in your inner circle. This knowledge can prove invaluable for both prevention and a rapid response should you experience this medical condition.
The autonomic nervous system: what happens with AD
The autonomic nervous system is like a control center in your body. This vital system carefully manages key body functions by sending signals through the spinal cord. These messages go back and forth between your brain and body to help regulate and control blood pressure, heart rate, temperature regulation, digestion, sweating, sexual function, and dilation of your eyes.
Autonomic dysreflexia is what doctors consider an abnormal response by the autonomic nervous system triggered by a variety of events happening in your body. These causes of autonomic dysreflexia range widely in seriousness and nature—ingrown toenails, tight-fitting clothing, kidney stones, constipation, or even sexual activity.
Normally the body responds to stimuli from various triggers automatically or involuntarily, so it's not something you have to think about. But when you have a spinal cord injury, your body's response to what is happening goes unnoticed by you. These automatic messages to your brain can't travel through the spinal cord corridor due to the damage.
So autonomic dysreflexia is like your body's backup plan. It is a way of letting you know something is happening or there is an issue by increasing your blood pressure.
Who is at risk for autonomic dysreflexia?
Your vulnerability to this serious medical condition will vary depending on the location—as well as severity—of your spinal cord injury. (Your medical team likely informed you of the location of the injury using spinal cord medical labels, such as the letter T followed by a number.)
If your injury is:
· At T6 or above, you may be at high risk for autonomic dysreflexia
· From T6 to T10, you may be at moderate risk for this issue
· Below T10, you are not at risk for autonomic dysreflexia
What you can do about autonomic dysreflexia
Now that you know a little more about this potentially life-threatening issue, it's important that you look out for symptoms of autonomic dysreflexia so that you and your helpers can respond quickly.
Also, make sure your medical team is knowledgeable about this condition if you fall under the high- or moderate-risk categories. In the event of a medical emergency, the Christopher and Dana Reeve Foundation offers a downloadable and printable autonomic dysreflexia wallet card that may be helpful to your physician or ER doctor.